Covid measures present new measles risk
While dealing with the Covid-19 crisis reduced the prevalence of other communicable diseases, like measles, they also interrupted the delivery of vaccines against such illnesses. A lack of supplies meant vaccines were unavailable in some countries.
In a nutshell
- Anti-pandemic measures have reduced measles cases
- They have also interrupted immunization programs
- A measles outbreak could be looming
With much of the world engaged in some degree of social distancing to avoid exposure to Covid-19, health officials are documenting a dramatic reduction in the prevalence of other infectious diseases, measles foremost among them. The respite will be short-lived. The stress of Covid-19 on medical resources is disrupting measles vaccine delivery for tens of millions of children in dozens of countries, increasing the risk of future deadly outbreaks worldwide.
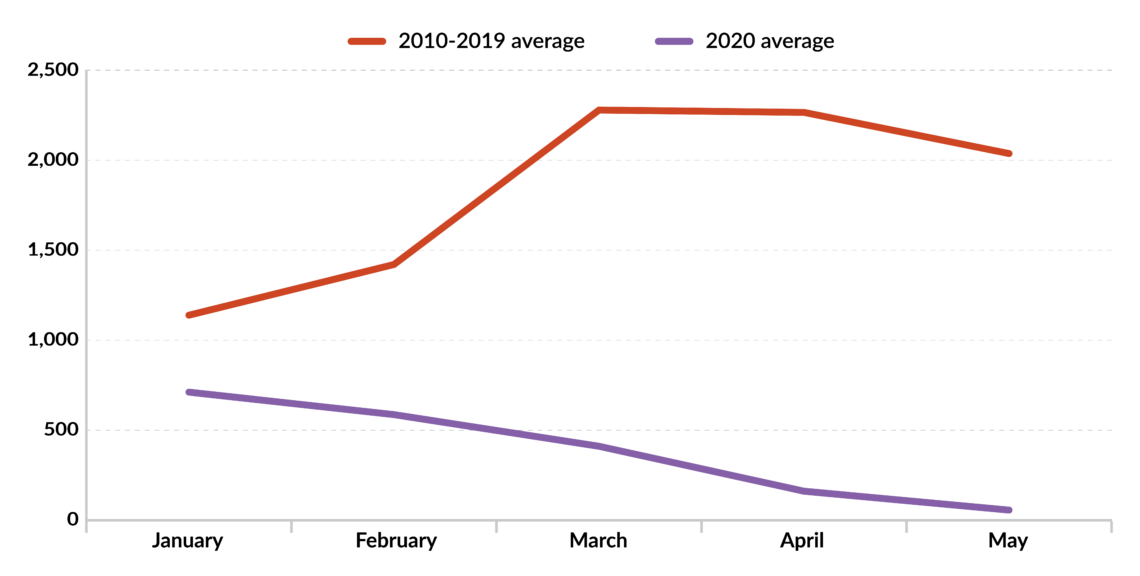
Much like the coronavirus that causes Covid-19, the measles virus (morbillivirus) is transmitted through airborne respiratory droplets, or by the nasal and throat secretions of those infected. The closure of schools and the seclusion of many families is greatly reducing individuals’ exposure to measles contagion. The 1,917 cases reported to the European Center for Disease Prevention and Control (January 2020 through May 2020) was the second-lowest number during peak measles season in the past decade.
Researchers also reported that cases in 2020 sharply decreased for the first time as the peak season progressed, even in countries with the highest number of infections (Belgium, Bulgaria, Germany, Spain, France, Italy, Romania and the United Kingdom). The number of cases in these countries in May was also the lowest recorded since 2010.
Progress threatened
The decline in cases certainly qualifies as a benefit in the Covid-19 calculation, but it is heavily outweighed by the costs of foregone inoculations that threaten to reverse years of advances in measles control and eradication.
Prior to the introduction of the measles vaccine, the disease resulted in an estimated 2.6 million deaths annually.
According to the World Health Organization (WHO), some 86 percent of the world’s children in 2018 received one dose of measles vaccine by their first birthday – up from 72 percent in 2000. Because a single dose typically fails to confer immunity in about 15 percent of children, two doses of the vaccine are recommended – which an estimated 69 of children received in 2018.
Prior to the introduction of the measles vaccine, in 1963, the disease resulted in an estimated 2.6 million deaths annually. Despite a variety of mass inoculation programs, more than 10 million cases of measles and 140,000 measles deaths worldwide were reported in 2018 – mostly among children under the age of five.
Vaccine disruption
It is virtually certain that those tragic numbers will worsen soon given recent diminished vaccine access and the disruption of immunization programs. The WHO declared Covid-19 a pandemic on March 11, 2020, and thereafter recommended postponing mass immunization campaigns in countries without active outbreaks of vaccine-preventable diseases. Officials were concerned that the large groups that assemble for inoculation would exacerbate the spread of Covid-19. In this instance, however, the cure could be much worse than the disease.
All told, 37 low-income and middle-income countries suspended mass immunization activities, thereby subjecting an estimated 117 million children to a greater risk of measles infection.
Facts & figures

The stress of Covid-19 on vaccine supply chains and healthcare delivery is further limiting immunizations. Researchers have documented vaccine shortages in 21 developing countries where limited resources are being allocated to treatments for Covid-19.
A resurgence of measles would also invite a host of other health threats – particularly among children without adequate nutrition and healthcare. The disease suppresses the immune system, which increases their vulnerability to a variety of secondary conditions such as ear infections, diarrhea, encephalitis and pneumonia. All of these are associated with substantial morbidity and mortality, according to the United States Centers for Disease Control and Prevention.
‘Notable decrease’
Declines in both vaccine supply and immunizations are not limited to developing countries; even the U.S. is experiencing Covid-related vaccine disruptions. Faced with rapidly rising numbers of coronavirus patients, hospitals and clinics have been postponing routine preventive and other nonemergency care since March. At the same time, some 43 states issued social distancing mandates and travel restrictions that deter well-child visits. Parents’ fears about Covid-19 exposure at doctors’ offices and health clinics also discourage such visits.
Based on data from the U.S. government’s Vaccine Tracking System, researchers have documented a “notable decrease” in both orders for the measles vaccine and administration of the vaccine during the four-month peak measles seasons in 2019 and 2020 (January-April). The 2020 decline started a week after President Donald Trump declared Covid-19 a national emergency on March 13, 2020.
The number of measles, mumps, and rubella vaccines delivered in England declined by 20 percent during the first three weeks of the Covid-19 lockdown.
Similarly, reviewing data submitted by 1,000 U.S. pediatricians, the electronic health records company PCC documented a 50 percent decline in measles vaccinations from February 16, 2020 to April 5, 2020. The number of measles, mumps, and rubella (MMR) vaccines delivered in England declined by 20 percent during the first three weeks of the Covid-19 lockdown, according to London’s Imperial College Child Health Unit. Declines were likewise reported in Scotland.
Professor Sonia Saxena, who leads Imperial College’s Child Health Unit, said parents are postponing immunizations out of concern about overburdening the National Health Service (NHS) amid the Covid-19 crisis, as well as risking exposure during a clinic visit. “Vaccines are a priority for GP surgeries, yet we are seeing this messaging has been lost,” she said. “Instead, the dominant message is everyone should stay at home and avoid burdening the NHS.”
Dangerous complacency
Despite pre-Covid-19 progress in the fight to eradicate measles, outbreaks began increasing in 2018. The WHO reported a 30 percent increase in measles cases globally that year. Moreover, 98 countries reported more cases of measles in 2018 than in 2017, contributing to an upsurge that UNICEF characterized as “alarmingly high levels.”
A variety of factors contributed to the resurgence, but the primary cause is what public health officials call “vaccine hesitancy” – defined by the WHO as “the reluctance or refusal to vaccinate despite the availability of vaccines.” Indeed, the organization has repeatedly ranked vaccine hesitancy among its 10 threats to global health. The irony is that widespread vaccination and the immunity it confers has nurtured a dangerous degree of complacency about the risks of disease outbreaks.
Even in countries where measles has been officially eradicated, the eradication is inherently unstable and dependent on maintaining very high rates of immunization. But a steady accumulation of unvaccinated individuals erodes the “herd immunity threshold,” or the proportion of people who must be vaccinated to prevent outbreaks. The minimum threshold, scientists say, is a vaccination rate of 90 percent.
In response to the decline in inoculations related to Covid-19, public health officials are calling for urgent action to prevent a wave of deadly measles outbreaks in the near future. But that is easier said than done when the most vulnerable populations are in countries lacking medical resources and reliable healthcare infrastructure.
Compared to Covid-19, the potential for lives lost to measles is alarming to contemplate.






